A new pilot program will bring a model for opioid addiction treatment pioneered in Bangor to communities across the state beginning next week.
The pilot, which will last for a year, will use state funding to expand opioid treatment across Maine using a model developed by Penobscot Community Health Care at its Bridge Clinic in Bangor that’s aimed at making treatment more accessible. It will spread the model across Maine, especially into rural areas that have been some of the hardest hit by the opioid epidemic.
The program, a collaboration between the Maine Primary Care Association and PCHC, arrives as 2021 is primed to be Maine’s most deadly year for overdoses on record. While the program was about three years in the making, beginning before the COVID-19 pandemic hit Maine in March of 2020, the people who helped make it happen acknowledged Wednesday that the pandemic was making treatment more necessary than ever.
The Bridge Clinic, which opened two and a half years ago, offers medication-assisted treatment that is low barrier, meaning the clinic serves people who might have difficulty getting help otherwise. Since it began, it has treated hundreds of people who likely would not have been treated, said PCHC Chief Medical Officer Noah Nesin. The clinic prescribes Suboxone — an anti-addiction medication with buprenorphine and naloxone — quickly to people interested in starting treatment, sees them weekly and tries to enroll them in more traditional recovery programs that involve counseling.
Some of the people the clinic has helped include those who don’t have reliable transportation, were recently released from jail and have been unsuccessful in other opioid treatment programs.
“These are, by the way, the people with the most severe disease — the people with the greatest risk of dying,” Nesin said. “That’s why this matters.”
Staff from PCHC and the Maine Primary Care Association will train staff from six of Maine’s 20 community health centers on developing opioid treatment programs modeled after the Bridge Clinic. The work will be done according to the ECHO model used in health care in which one organization teaches a successful treatment model to other entities, which then create their own organic models.
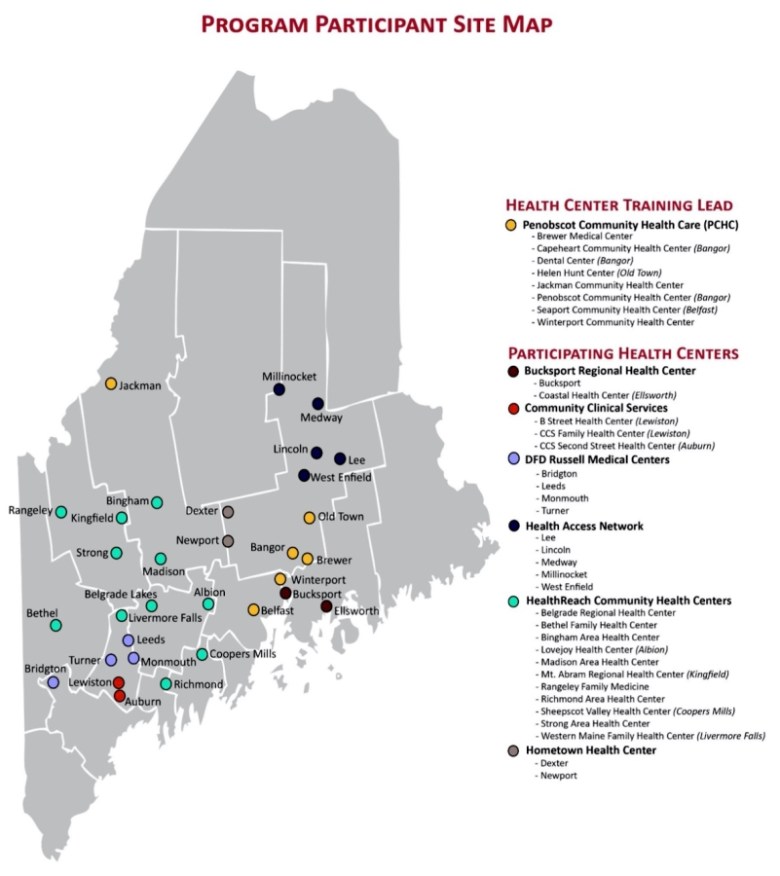
Those health centers have 27 total locations spread across 10 of Maine’s 16 counties with patients that make up about 65 percent of those served by community health centers across the state. The centers are located in Androscoggin, Cumberland, Franklin, Hancock, Kennebec, Lincoln, Oxford, Penobscot, Sagadahoc and Somerset counties.
Gordon Smith, director of Maine’s opioid response in the office of Gov. Janet Mills, who was involved in the effort, noted that it was vital for locations across Maine to have a quick and effective treatment available to those with opioid use disorder.
“This effort is a very important step to see if we can expand the work Penobscot Community Health Care has done in the Bangor area,” Smith said.
Advocates had previously tried to spearhead such a program with legislation, Sen. Ned Claxton, D-Auburn, noted, though it did not pass in the legislative session that ended last year.
While genetic factors can be involved in opioid use disorder, Smith said people’s opioid use is often a reaction to various traumatic events in their lives. Many of those affected are some of the most at-risk people in the state, he said.
Nesin, who primarily oversees patients in Penobscot County, noted that the increased prevalence of fentanyl in street drugs, combined with the increasing isolation brought by the pandemic, had combined to make situation that was deadly pre-pandemic worse.
“It’s really a difficult time everywhere,” said Smith, though he did note the expansion in the availability of the anti-overdose drug naloxone. “But, particularly, Penobscot County has seen a much greater increase per capita than, for instance, the increase seen in Cumberland County.”
Participating organizations are Bucksport Regional Health Center; Lewiston-based Community Clinical Services; DFD Russell Medical centers, which has locations in Leeds, Turner, Monmouth and Bridgton; Lincoln-based Health Access Network; HealthReach Community Health Centers with 11 locations across the state; and Newport-based Hometown Health Center.



